Neck pain is quite possibly one of the most common complaints when it comes to doctor visits for disorders of the spine. The portion of the back bone that involves the neck is referred to as the cervical spine. Problems in the neck due to compressed disc, degenerative disc disease, or other conditions may require surgical intervention in order for the patient to achieve relief of associated symptoms. Cervical fusion involves the stabilization of vertebrae in the neck.
Medical Advances
In the past, open surgery was required in order to perform a fusion of the cervical spine. This requires a fairly large incision and disruption of muscle and connective tissue in order to reach the cervical spine. Cutting and retraction are typically required and may result in increased pain. Once any affected tissue is removed, the surgeon can perform a bone graft with natural or artificial bone tissue. Natural tissue can come from the patient or another source. The bone graft is done to encourage bone growth to fuse vertebrae and better stabilize the neck. The latest advances in technology allow for minimally invasive options when it comes to surgery of the spine.
In most cases, minimally invasive cervical fusion can shorten the duration of healing time while reducing painful recovery for most patients. Lower rates of post-operative infection are also considered to be a benefit of minimally invasive surgical options. Patients may have less blood loss, spend less time in the hospital, and may feel better more quickly than with traditional surgical methods.
Approaches
While open surgery is sometimes the best option for certain circumstances, many patients will be good candidates for less invasive cervical fusion surgeries. There are several techniques that can be used that are less invasive for the patient. Some minimally invasive cervical fusion procedures only require an incision of about an inch. This requires less disruption of structures and soft tissues in the area. Many procedures can also be performed on an outpatient bases, reducing overall costs for the patient.
Anterior cervical fusion involves placement of the bone graft at the front of the neck rather than the posterior, or back. This involves the cutting of only one muscle and a clear view of the entire surgical spine for the surgeon. Because the surgeon has easier access to the cervical spine, lower rates of surgical site infection are also noted with an anterior approach over the posterior approach.
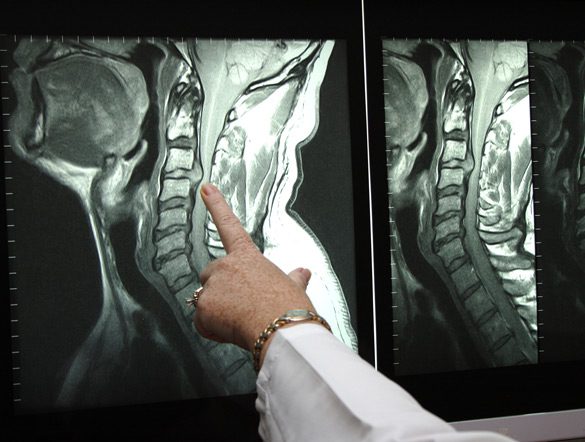
With the use of new technology, surgeons can use special x-rays during surgical procedures to direct the tools and placement of hardware or bone grafts using minimal incision and no disruption of tissue. Surgeons can avoid potential issues of working around the esophagus and vital blood vessels with the implementation of a cervical pedicle screw. Because the surgeon can see inside of the body through the use of x-rays, a wire can be placed at the optimal site location and through the proper trajectory to guide placement of surgical tools and hardware to the best location to provide optimal support and healing.

